469 results
347 Aerodynamic Size Distribution of SARS-CoV-2 Aerosol Shedding
- Part of
- Kristen K. Coleman, Petri Kalliomäkia, Jianyu Lai, S.-H. Sheldon Tai, Jennifer German, Filbert Hong, Barbara Albert, Yi Esparza, Aditya K. Srikakulapu, Maria Schanz, Alycia Ann Smith, Isabel Sierra Maldonado, Molly Oertela, Naja Fadula, Arantza Eiguren-Fernandez, Gregory S. Lewis, Kathleen M. McPhaul, Donald K. Milton
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 105
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: We designed the Biocascade Exhaled Breath Sampler (BEBS) to characterize viral aerosol shedding among individuals with influenza and other respiratory virus infections. We first aimed to test the BEBS on volunteer COVID-19 cases and report the aerodynamic size distribution of exhaled breath aerosol particles carrying SARS-CoV-2 RNA. METHODS/STUDY POPULATION: From June 15 through December 15, 2022, we recruited 27 PCR-confirmed COVID-19 cases from a college campus and the surrounding community to provide 30-minute breath samples into a well-validated Gesundheit-II (G-II) exhaled breath aerosol sampler. Among these individuals, 17 provided an additional exhaled breath sample into the newly designed BEBS. We quantified samples for viral RNA using reverse transcription digital polymerase chain reaction (RT-dPCR) and determined the viral RNA copies collected within two aerosol size fractions (≤5 µm and >5 µm in diameter) from the G-II, and four aerosol size fractions (<1.15 µm, 1.15–3.2 µm, 3.3–8.2 µm, and >8.2 µm) from the BEBS. RESULTS/ANTICIPATED RESULTS: Individuals with a SARS-CoV-2 Omicron BA.4 or BA.5 infection shed virus in aerosols at an average rate of 7.5x103 RNA copies per 30-minute G-II sample, with 78% of the total RNA in aerosols ≤5 µm in diameter. Among the BEBS samples, 10% of the total viral RNA was detected in aerosols <1.15 µm, 43% in 1.15–3.2 µm, 37% in 3.3–8.2 µm, and 10% in the >8.2 µm size fraction. Based on viral RNA loads, our results indicate that exhaled aerosols ≤3.2 µm contribute the majority of SARS-CoV-2 inhalation exposure. DISCUSSION/SIGNIFICANCE: Our data provide additional evidence that respirable aerosols contribute to the spread of SARS-CoV-2. Thus, our data suggest that mitigation measures designed to reduce infectious aerosol inhalation, such as ventilation and the use of air cleaners and respirators, are needed to control the spread.
Inequality on the frontline: A multi-country study on gender differences in mental health among healthcare workers during the COVID-19 pandemic
- Diana Czepiel, Clare McCormack, Andréa T.C. da Silva, Dominika Seblova, Maria F. Moro, Alexandra Restrepo-Henao, Adriana M. Martínez, Oyeyemi Afolabi, Lubna Alnasser, Rubén Alvarado, Hiroki Asaoka, Olatunde Ayinde, Arin Balalian, Dinarte Ballester, Josleen A.l. Barathie, Armando Basagoitia, Djordje Basic, María S. Burrone, Mauro G. Carta, Sol Durand-Arias, Mehmet Eskin, Eduardo Fernández-Jiménez, Marcela I. F. Frey, Oye Gureje, Anna Isahakyan, Rodrigo Jaldo, Elie G. Karam, Dorra Khattech, Jutta Lindert, Gonzalo Martínez-Alés, Franco Mascayano, Roberto Mediavilla, Javier A. Narvaez Gonzalez, Aimee Nasser-Karam, Daisuke Nishi, Olusegun Olaopa, Uta Ouali, Victor Puac-Polanco, Dorian E. Ramírez, Jorge Ramírez, Eliut Rivera-Segarra, Bart P.F. Rutten, Julian Santaella-Tenorio, Jaime C. Sapag, Jana Šeblová, María T. S. Soto, Maria Tavares-Cavalcanti, Linda Valeri, Marit Sijbrandij, Ezra S. Susser, Hans W. Hoek, Els van der Ven
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 11 / 2024
- Published online by Cambridge University Press:
- 04 March 2024, e34
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Healthcare workers (HCWs) were at increased risk for mental health problems during the COVID-19 pandemic, with prior data suggesting women may be particularly vulnerable. Our global mental health study aimed to examine factors associated with gender differences in psychological distress and depressive symptoms among HCWs during COVID-19. Across 22 countries in South America, Europe, Asia and Africa, 32,410 HCWs participated in the COVID-19 HEalth caRe wOrkErS (HEROES) study between March 2020 and February 2021. They completed the General Health Questionnaire-12, the Patient Health Questionnaire-9 and questions about pandemic-relevant exposures. Consistently across countries, women reported elevated mental health problems compared to men. Women also reported increased COVID-19-relevant stressors, including insufficient personal protective equipment and less support from colleagues, while men reported increased contact with COVID-19 patients. At the country level, HCWs in countries with higher gender inequality reported less mental health problems. Higher COVID-19 mortality rates were associated with increased psychological distress merely among women. Our findings suggest that among HCWs, women may have been disproportionately exposed to COVID-19-relevant stressors at the individual and country level. This highlights the importance of considering gender in emergency response efforts to safeguard women’s well-being and ensure healthcare system preparedness during future public health crises.
5 Cognitive Rehabilitation Using Teleneuropsychology. A Cohort Study in South America
- Carlos Martinez Canyazo, Rodrigo S Fernandez, Maria B Helou, Micaela Arruabarrena, Nicolas Corvalan, Agostina Carello, Paula Harris, Monica Feldman, Ismael Luis Calandri, Maria E Martin, Ricardo F Allegri, Lucia Crivelli
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, p. 209
-
- Article
-
- You have access Access
- Export citation
-
Objective:
The COVID-19 pandemic has affected the continuity of cognitive rehabilitation (CR) worldwide. However, the use of teleneuropsychology (TNP) to provide CR has contributed significantly to the continuity of treatment. The objective of this study was to measure the effects of CR via the TNP on cognition, neuropsychiatric symptoms, and memory strategies in a cohort of patients with Mild Cognitive Impairment (MCI).
Participants and Methods:A sample of 60 patients (60% female; age: 72.4±6.96) with MCI according to Petersen criteria was randomly divided into two groups: 30 cases (treatment group) and 30 controls (waiting list group). Subjects were matched for age, sex, and MMSE or MoCA.
The treatment group received ten weekly CR sessions of 45 minutes weekly. Pre-treatment (week 0) and post-treatment (week 10) measures were assessed for both groups. Different Linear Mixed Models were estimated to test treatment effect (CR vs. Controls) on each outcome of interest over Time (Pre/Post), controlling for Diagnosis, Age, Sex, and MMSE/MoCA performance.
Results:A significant Group (Control/Treatment) x Time (pre/post) interaction revealed that the treatment group at 10 weeks had better scores in cognitive variables: memory (RAVLT learning trials p=0.030; RAVLT delayed recall p=0.029), phonological fluency(p=0.001), activities of daily living (FAQ p=0.001), satisfaction with memory performance (MMQ Satisfaction p=0.004) and use of memory strategies (MMQ Strategy p=0.00), and a significant reduction of affective symptomatology: depression (GDS p=0.00), neuropsychiatric symptoms (NPIQ p=0.045), Forgetfulness (EDO-10 p=0.00), Stress (DAS Stress p=0.00).
Conclusions:This is the first study to test CR using teleNP in South America. Our results suggest that CR through teleNP is an effective intervention to improve performance on cognitive variables and reduce neuropsychiatric symptomatology compared to patients with MCI. These results have great significance in the context of the COVID-19 pandemic in South America, where teleNP is proving to be a valuable tool.
Ten New Insights in Climate Science 2023/2024
- Mercedes Bustamante, Joyashree Roy, Daniel Ospina, Ploy Achakulwisut, Anubha Aggarwal, Ana Bastos, Wendy Broadgate, Josep G. Canadell, Edward R. Carr, Deliang Chen, Helen A. Cleugh, Kristie L. Ebi, Clea Edwards, Carol Farbotko, Marcos Fernández-Martínez, Thomas L. Frölicher, Sabine Fuss, Oliver Geden, Nicolas Gruber, Luke J. Harrington, Judith Hauck, Zeke Hausfather, Sophie Hebden, Aniek Hebinck, Saleemul Huq, Matthias Huss, M. Laurice P. Jamero, Sirkku Juhola, Nilushi Kumarasinghe, Shuaib Lwasa, Bishawjit Mallick, Maria Martin, Steven McGreevy, Paula Mirazo, Aditi Mukherji, Greg Muttitt, Gregory F. Nemet, David Obura, Chukwumerije Okereke, Tom Oliver, Ben Orlove, Nadia S. Ouedraogo, Prabir K. Patra, Mark Pelling, Laura M. Pereira, Åsa Persson, Julia Pongratz, Anjal Prakash, Anja Rammig, Colin Raymond, Aaron Redman, Cristobal Reveco, Johan Rockström, Regina Rodrigues, David R. Rounce, E. Lisa F. Schipper, Peter Schlosser, Odirilwe Selomane, Gregor Semieniuk, Yunne-Jai Shin, Tasneem A. Siddiqui, Vartika Singh, Giles B. Sioen, Youba Sokona, Detlef Stammer, Norman J. Steinert, Sunhee Suk, Rowan Sutton, Lisa Thalheimer, Vikki Thompson, Gregory Trencher, Kees van der Geest, Saskia E. Werners, Thea Wübbelmann, Nico Wunderling, Jiabo Yin, Kirsten Zickfeld, Jakob Zscheischler
-
- Journal:
- Global Sustainability / Accepted manuscript
- Published online by Cambridge University Press:
- 01 December 2023, pp. 1-58
-
- Article
-
- You have access Access
- Open access
- Export citation
The Pharmaceutical Market for Biological Products in Latin America: A Comprehensive Analysis of Regional Sales Data
- Esteban Ortiz-Prado, Juan S. Izquierdo-Condoy, Jorge Eduardo Vasconez-González, Gabriela Dávila, Trigomar Correa, Raúl Fernández-Naranjo
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 51 / Issue S1 / Fall 2023
- Published online by Cambridge University Press:
- 29 December 2023, pp. 39-61
- Print publication:
- Fall 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The global market for biologics and biosimilar pharmaceutical products is experiencing rapid expansion, primarily driven by the continuous discovery of new molecules. However, information regarding Latin America’s biological market remains limited.
Archaeological Analysis of a Water Mill from the Nineteenth Century in Salta, Argentina
- Pablo José Pifano, Fernando J. Fernández, Ailín A. Guillermo, Natalia S. Petrucci, María C. Páez
-
- Journal:
- Latin American Antiquity , First View
- Published online by Cambridge University Press:
- 31 August 2023, pp. 1-17
-
- Article
- Export citation
-
Hydraulic mills were introduced in the early colonial period in the Americas to grind wheat into flour. During the nineteenth and twentieth centuries, the rise of the agro-export model in Latin America shaped the development of a flour industry in which water-powered mills played a central role. Over time, these technologies were used not only to increase production for the export market but also to meet the needs of domestic consumption, both local and regional. In this context, in 2017 we began to investigate the characteristics of a hydraulic mill, currently in disuse, in the town of Payogasta in the province of Salta (Argentina), to determine its chronology and functionality. In addition to surveying the structure, we conducted excavations in the nearby rooms that were part of the site. We found that this mill was in operation between the end of the nineteenth and the end of the twentieth centuries, grinding wheat, corn, carob, and red bell pepper, and that the adjoining rooms were used to house the people who were waiting their turn to grind their raw materials.
Night-time/daytime Protein S100B serum levels in paranoid schizophrenic patients
- E. Diaz-Mesa, A. Morera-Fumero, L. Torres-Tejera, A. Crisostomo-Siverio, P. Abreu-Gonzalez, R. Zuñiga-Costa, S. Yelmo-Cruz, R. Cejas-Mendez, C. Rodriguez-Jimenez, L. Fernandez-Lopez, M. Henry-Benitez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S445-S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
S100B is a calcium-binding astrocyte-specific cytokine, that is considered a biomarker of neurodegeneration; which may be involved in the imbalance of the inflammatory response observed in several brain disorders, including major depression and schizophrenia. Two meta-analyses have reported higher serum levels of S100B in patients with schizophrenia respect to healthy controls.
Different studies have described circadian and seasonal variations of biological variables, such as melatonin or cortisol. It has been reported that there is not circadian rhythm of S100B blood levels in healthy subjects. However, it is not known whether there are circadian oscillations in S100B blood concentrations in patients with schizophrenia.
ObjectivesThe aim of this study is to describe S100B serum levels in patients with schizophrenia and to analyse whether they follow a circadian rhythm.
MethodsOur sample consists in 47 patients in acute phase and stabilized status. Blood samples were collected at 12:00 and 00:00 hours by venipuncture. Serum levels of Protein S100B were measured three times: at admission, discharge and three months after discharge. Protein S100B was measured by means of ELISA (Enzyme-linked immunosorbent assay) techniques.
Results12:00 24:00 P ADMISSION 132,95±199,27 85,85±121,44 0,004 DISCHARGE 73,65±71,744 75,80±123,628 0,070 CONTROL 43,49±34,60 40,14±23,08 0,47 P global P Admission Vs. Discharge P Admission Vs. Control P Discharge Vs. Control 0,97 There is a significance difference between 12:00 and 24:00 at admission for the Protein S100B.However, these difference did not occur at discharge and at three months after discharge.It can be interpreted as there is a circadian rhythm of Protein S100B when the patient has got a psychotic outbreak and disappears at discharge and when is psychopathologically stable.
ConclusionsWith respect to our results we can hypothesize that schizophrenic patients in acute relapse present circadian S100B rhythm that is not present when the patients are clinically stable.Furthermore, the decrease of serum protein S100B levels at discharge is indicative of a reduction of the cerebral inflammation, thus it can be a biomarker of cerebral inflammation and this reduction can be the effect of the treatment. Finally, its circadianity could be a guide of this process and clinical improvement.
Disclosure of InterestNone Declared
PSYCHIATRIC COMORBIDITY IN A SAMPLE OF PATIENTS WITH COGNITIVE-BEHAVIORAL MINORITY DISEASE
- R. De la Mata, C. Manso-Bazús, S. Pujol, L. Torrent, L. Urraca, D. Vázquez-Tarrio, M. Esteve, E. Fernández, M. Pàmias
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S743
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
About the term cognitive-behavioral minority disease or rare disease are a group of diseases that affect between 6-8% of the populatio. It is estimated that there are more than 7000 in the world, the majority with a genetic basis and affect various organs and systems, they also present psychiactric comorbidities and cause a physical or mental disability. Given its definition, it is difficult to see a large number of these patients in our usual clinical activity, so their management can be complicated.
ObjectivesTo evaluate the prevalence of psychiatric comorbidity and the prevalence of psyhcopharmacological treatment in children and adolescents whe present a minority disease.
MethodsThis is a descriptive, controlled, retrospective cross-sectional study of a sample obtained by non-probabilistic sampling, which is representative of the study population.
The statistical analysis was made using the statistical program SPSS V22 (2013).
ResultsWith a sample of 114 patients, of which 26,6% presented fragile X syndrome, secondly 25,3% presented Prader-Willi Syndrome and 48,1% other chromosomal abnormalities.
By subgroups (male:female): in Prader-Willi syndrome 6:14 (30%:70%), in Fragile X syndrome 12:9 (57,14%: 42,86%) and in other diseases 25:13 (75,69%: 34,21%).
ConclusionsThe creation of clinical expert units makes the possibility to increase knowledge of diseases whose prevalence in the population, thanks to technological advances, is increasing and where scientific knowledge is still limited.
These units are also important, in order to be able to offer personalized intensive treatments in order to reduce polypharmacy. There is not a great difference between the minority diagnosis and polypharmacy, although there is less polypharmacy than expected, which may be the result of the success of the most intensive and personal psychotherapeutic intervention in the unit.
Disclosure of InterestNone Declared
Do attention-deficit/hyperactivity symptoms influence treatment outcome in gambling disorder?
- C. Vintró-Alcaraz, G. Mestre-Bach, R. Granero, M. Gómez-Peña, L. Moragas, F. Fernández-Aranda, M. N. Potenza, S. Jiménez-Murcia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S58-S59
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Numerous studies point to the comorbidity between gambling disorder (GD) and attention deficit hyperactivity disorder (ADHD). However, there is a lack of research exploring how ADHD symptoms might influence psychological treatment outcomes for GD.
ObjectivesTherefore, we aimed to explore differences between patients with GD with and without ADHD symptoms regarding psychopathology, personality, sociodemographic and especially treatment outcome measures.
MethodsThis longitudinal study included n=170 patients with GD receiving 16 sessions of cognitive behavioral therapy (CBT) in a specialized unit of a public hospital. Multiple self-reported instruments were used to assess GD severity, personality, ADHD and other symptoms and sociodemographic measures prior to treatment.
ResultsA clinical profile characterized by greater GD severity, higher psychopathology and impulsivity, and less adaptive personality features was observed in patients with self-reported ADHD symptoms compared to those without. No significant differences in treatment response (measured by dropout and relapse rates) were reported between the two groups. However, patients with ADHD symptoms described more severe relapses (more money gambled) and GD patients who relapsed scored higher on measures of ADHD, particularly inattention.
ConclusionsIndividuals with GD and ADHD may experience more severe relapses following treatment, suggesting a need for more vigilant follow-up and interventions for patients with this comorbidity.
Disclosure of InterestC. Vintró-Alcaraz: None Declared, G. Mestre-Bach: None Declared, R. Granero: None Declared, M. Gómez-Peña: None Declared, L. Moragas: None Declared, F. Fernández-Aranda Consultant of: Novo Nordisk and editorial honoraria as EIC from Wiley, M. Potenza Consultant of: Opiant Pharmaceuticals, Idorsia Pharmaceuticals, AXA, Game Day Data, Baria-Tek and the Addiction Policy Forum; has been involved in a patent application with Yale University and Novartis; has received research support (to Yale) from Mohegan Sun Casino and Connecticut Council on Problem Gambling; and has consulted for and/or advised gambling and legal entities on issues related to impulse-control/addictive disorders, S. Jiménez-Murcia: None Declared
Time discrimination in psychosis: findings from a neuroimaging study
- J. Goena, C. Vidal, S. Solís, M. Fernandez Seara, F. Ortuño, S. Garcés, M. Fernández
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S130-S131
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Previous functional neuroimaging studies have demonstrated a brain network responsible of time discrimination (TD) processes, which may play a significant mediating role in other cognitive processes, such as change detection and cognitive control. The study of TD and its dysfunction in psychosis has become a matter of growing interest. We hypothesize that the impairment of the TD network is involved both in the mechanisms of psychosis and in the cognitive deficit presented by patients.
Objectives1. To delimit the brain regions involved in TD.
2. To examine the dysfunction in TD brain network in patients diagnosed with psychosis.
3. To sudy the integrity of brain white matter pathways in psychosis.
4. To verify whether the neuroimaging findings and TD test performance predict the neurocognitive profile of the patients.
MethodsParticipants included 20 patients with psychosis (PSY group) and 13 healthy controls (HC group). PSY group participants met remission criteria for 6 months prior to the study. Participants were interviewed for sociodemographic information and clinical assessments. They underwent a detailed cognitive assesment using the Measurement and Treatment Research to Improve Cognition in Schizophrenia (MATRICS) Consensus Cognitive Battery (MCCB). Neuroimaging study was performed on a 3 Tesla MRI scanner. We designed an experimental task including a test tool to assess TD and Oddbal detection (OD) paradigms with a cognitive control component. The task was conducted under functional magentic resonance imaging (fMRI). We used the general linear model analysis of the individual data of the fMRI images and the random effects model for group inference. Group differences in DTI were tested using tract-based spatial statistics (TBSS).
ResultsWe find statistically significant differences (fMRI) in the activity related to TD (in HC), with greater activity in frontal cortical regions, the insular cortex and the cerebellum. In the PSY group, differences in the functionality and activation pattern of brain networks responsible for TD are observed, although voxel clustering does not reach the cluster significance limit when compared to HC. Compared to the HC, the PSY group has a significant deficit of fractional anisotropy (DTI) in the whole brain and in 21 specific brain regions. The PSY group has significantly lower scores in six of the seven cognitive domains than the control group, as well as in the overall composite. We correlated FA values in the groups of interest with MCCB scores.
Image:
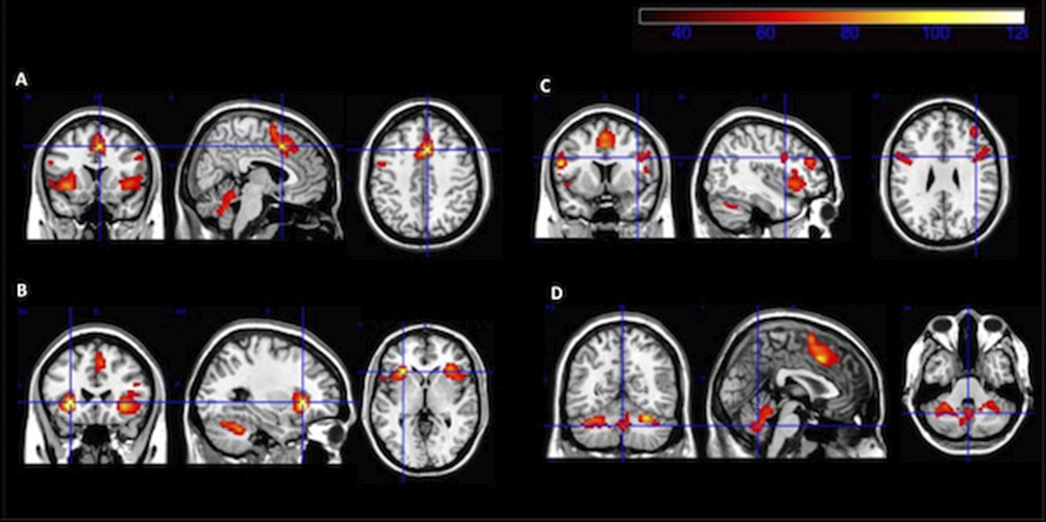
Image 2:
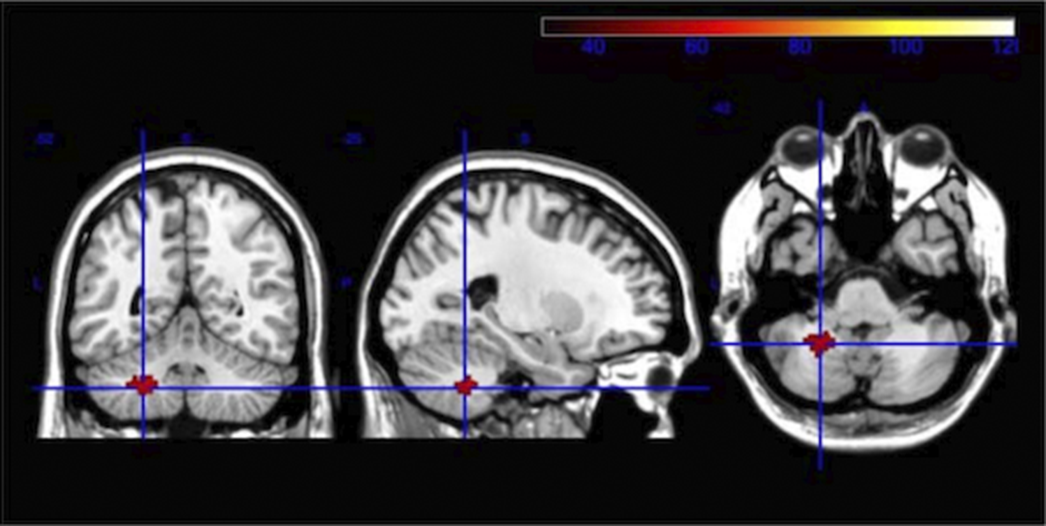
Image 3:
 Conclusions
ConclusionsWe have defined the TD network, its relationship with other brain networks and cognitive processes of more complexity. The inclusion of participants with stable psychosis allowed us to analyze de TD disfunction in the PSY group. We compared the integrity of TD related brain pathways and correlated the findings with various clinical characteristics and the cognitive impairment present in psychotic patients.
Disclosure of InterestNone Declared
A cross-sectional descriptive study to assess the impact of the “open door” policy on patient satisfaction
- M. Campillo, J. Marti, L. Rius, S. Garcia Fernandez, M. Olivero, G. Sanchez Tomico, G. Brusco-Passalaqua, E. Pechuan, T. Vates, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S910
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since the beginning of the modern psychiatry the acute units have established a “locked door” policy. Some studies show that this condition may increase patient’s discomfort and affect the perception of health quality of care (Boyer L, 2009, Eur Psychiatry Dec;24(8):540-9). Lately, several European countries such as Germany, Switzerland and Spain are starting to implement the “open-door” policy but its impact on patient’s satisfaction is still unknown (Hochstrasser, L, Frontiers in Psychiatry, 9(57). https://doi.org/10.3389/fpsyt.2018.00057) .
ObjectivesTo help characterize the advantages of the “open-door” policy implemented in an acute inpatient psychiatric unit in order to assess the patient’s view of it.
MethodsThis is a descriptive observational study carried out at an inpatient psychiatric unit. Data were collected after the implementation of the open door policy on June 2019, assessing the patient satisfaction of 31 subjects who completed the SATISPSY-22 scale at the time of discharge. Results are described using the average and its standard deviation.
ResultsResults show scores in all items above 50 points, being the care team and the quality of care the most valued ones with 82 and 79 points respectively. The overall score is above 65 points (Fig. 1).
Image:
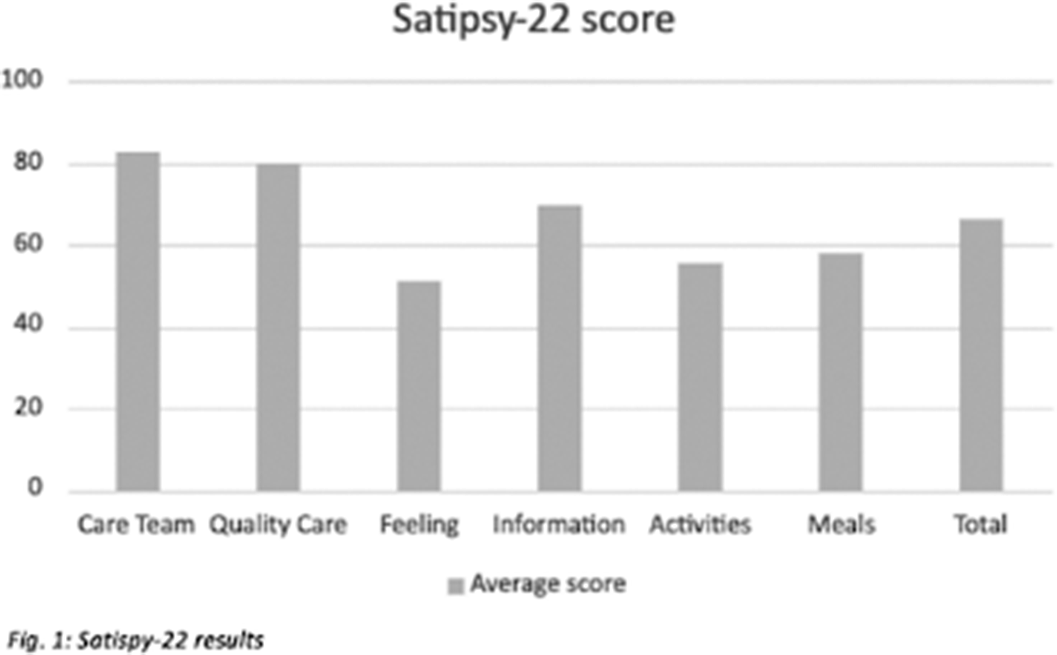 Conclusions
ConclusionsIn line with previous studies, our data suggests that the main impact of the “open-door” policy implementation is on patients’ perception of the care, being Quality of care and satisfaction with the Staff the items with highest scores. This could be explained by patients trusting more in the Care team, which would help enhance the therapeutic relationship improving therapeutic adherence, treatment adequacy and the outcome. Nevertheless, the Feeling related to hospitalisation was found to be the item with the lowest score. This could mean strategies should focus on improving patient’s insight regarding their clinical state and their need to be admitted. Our study supports the hypothesis that open-door policy in acute psychiatric units is seen positively by patients and that further research should be carried.
Disclosure of InterestNone Declared
Does intensive home treatment change treatment trajectories of psychiatric disorders?
- A. Martín-Blanco, A. González-Fernández, A. Farré, S. Vieira, P. Alvaro, C. Isern, D. Giménez, C. Torres, V. de la Cruz, C. Martín, N. Moll, O. Castro, M. Sagué-Vilavella
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S167-S168
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Intensive home treatment (IHT) for people experiencing a mental health crisis has been progressively established in many western countries as an alternative to in-ward admission. But is this a real alternative? We previously reported that patients treated in our IHT unit only differ from those voluntarily admitted to hospital in suicidal risk and severe behaviour disorders (not in other factors such as clinical severity) (Martín-Blanco et al., Rev Psiquiatr Salud Ment 2022;15:213-5). Now we are interested in disentangle if those patients who used to require inward management can be successfully treated at home.
ObjectivesTo describe subsequent treatment trajectories of the first 1000 admissions to our IHT unit and to compare clinical characteristics among the different groups of trajectories.
MethodsRetrospective cohort study. Subsequent treatment trajectories were collected from December 2016 to October 2022 and classified: absence, hospital, IHT, and mixed (hospital and IHT). Statistical significance was tested by means of ANOVA or Kruskal-Wallis test for quantitative variables (corrected for multiple comparisons) and chi-square tests for qualitative variables.
ResultsTables 1 shows the characteristics of the whole sample. Of the 1000 IHT admissions, 12.1% needed subsequent hospital admission(s), 12.7% IHT admission(s), and 9.3% mixed admission(s). There were no differences among these groups in median severity at IHT admission, but there were differences in the number of previous admissions (p=0.0001): the group with no subsequent admissions had less previous admissions than the other groups (pBonf<0.0001), and the group with subsequent IHT admissions had less than the group with mixed admissions (pBonf=0.0123). There were differences between groups regarding distribution of diagnoses (p<0.0001) (Fig. 1). When considering subsequent admissions by diagnosis, there were differences in severity at IHT admission (p=0.0068) and in number of previous hospitalizations (p<0.0001) (Fig. 2).
Table 1. Clinical characteristics of the whole sample (N=1000) mean SD Age (years) 47.07 17.02 CGI-s at admission * 5 4-5 N % Sex (female) 548 54.8% Psychotic disorders 463 46.3% Affective disorder 257 25.7% Bipolar disorder 128 12.8% Other disorders 152 15.2% Hospital admission in the previous 5 years 313 31.3% CGI-s: clinical global impression - severity. * median and IQR
Image:
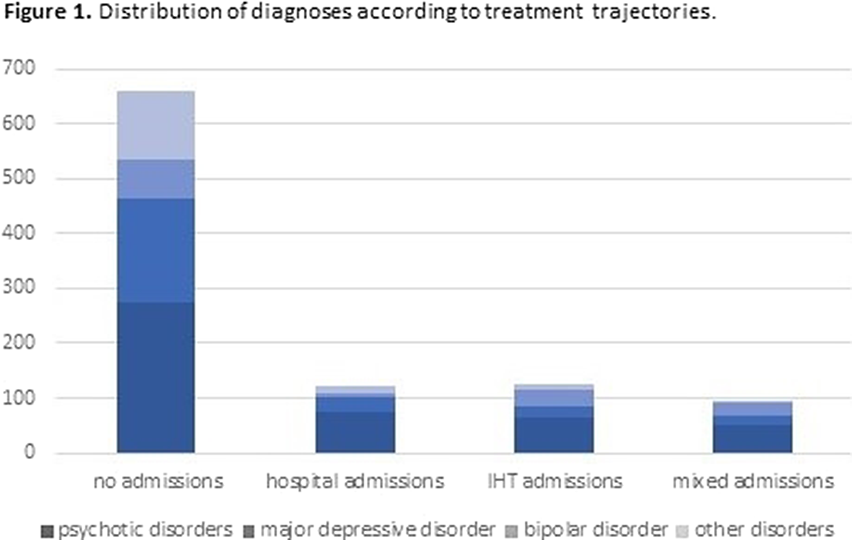
Image 2:
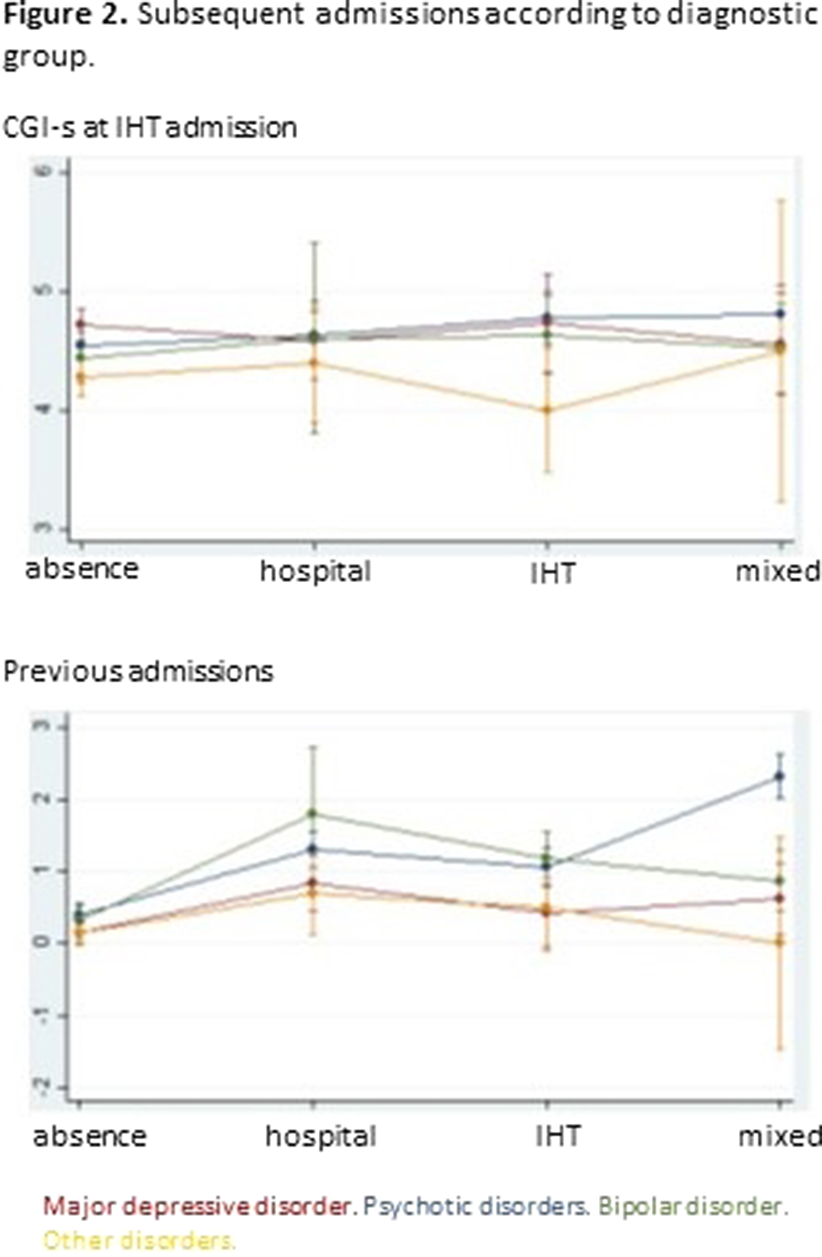 Conclusions
ConclusionsPatients that used to require inward management can now be treated at home when suffering an acute episode. Therefore, IHT has changed treatment trajectories for some patients with psychiatric disorders.
Disclosure of InterestNone Declared
Brief psychotic episode in an adult without medical antecedents after suffering the indirect consequences of the Russian-Ukrainian war
- R. G. Troyano, M. Fariña Francia, E. Marimon Muñoz, I. Fernandez Marquez, E. Miranda Ruiz, M. Arroyo Ucar, J. Ramirez Gonzalez, S. Ferreiro Gonzalez, C. Hidalgo, A. Quispe
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S911
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Almost nine months after the start of the war between Russia and Ukraine, millions of people have been affected physically, economically and mainly mentally. Those who have stayed in their homeland, and the ones that have chosen to emigrate to a safer place.
ObjectivesThe objective of this article is to assess the importance of social stressors in the onset of a brief psychotic episode, even in the absence of substance abuse or previous illnesses.
MethodsThe case of a 45-year-old woman is described, known by the Pediatric Emergency Service, for being the tutor of a patient who suffered from anxiety attacks, having emigrated without her parents from Ukraine together with her 5 brothers. The psychotic episode begins when our patient gets notified that she must abandon the custody of the girl, because she will have to go to Turkey with her legal guardians. The family explains the behavioral changes that the patient made and how the clinical picture worsened.
ResultsShe was admitted at the Hospital’s Psychiatry Service and antipsychotics treatment started. After 5 days, the episode had completely been solved.
ConclusionsIn conclusion, we highlight the importance of social problems in the development of a psychiatric pathology and the necessary elements to prevent it: family support network, fast and efficient care services and availability of hospital and pharmaceutical resources.
Disclosure of InterestNone Declared
Acute psychosis following corticosteroid administration for COVID-19 and Respiratory Syncytial Virus infection: A case study
- E. Miranda Ruiz, E. Marimon Muñoz, J. Ramirez Gonzalez, M. Fariña, R. G. Troyano, M. I. Arroyo Ucar, S. Ferreiro, I. Fernandez Marquez, C. Hidalgo, A. Quispe, L. Delgado
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S790
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Steroids are a necessary treatment for hypoxic respiratory failure; however there are many side effects that should be taken into account. A 44- year-old-woman with asthma and no past psychiatric history was admitted due to COVID-19 pneumonia and Respiratory syncytial virus (RSV) infection, presenting hypoxic respiratory failure. After two days of intravenous methylprednisolone administration, the patient presented acute psychosis and agitation.
It has been previously described that steroid use can cause effects such as mania, anxiety, agitation, delirium and psychosis amongst other. However they are a necessary treatment in respiratory illnesses and are sometimes unavoidable.
ObjectivesThe aim was to examine the appropriate medical response to steroid induced psychosis in patients with acute hypoxic failure.
MethodsA bibliographical review was done in PubMed database searching recent cases of steroid induced psychosis using the words (“Steroid”, “Psychosis” and “COVID-19”).
ResultsAccording to literature, it has been shown that partial or complete reduction of steroid use and/or use of psychotropic has been successfully used to treat steroid induced psychosis. Following the research it was decided to reduce intravenous methylprednisolone dose from 20mg/ 8h to 20mg/12h and start oral haloperidol 5mg/8h the first 24h and reducing the dose progressively as the patient recovered. After the first 24 hours the patient presented adequate response to steroids as well as partial response to antipsychotic treatment; presenting no further agitation, absence of hallucinations and partial persistence of the persecutory delusion. A couple of days later there was complete remission of the psychotic symptoms and the patient was on the way to recovery from COVID-19 and RSV.
ConclusionsThere is evidence that suggests that medications such as steroids used to treat COVID-19 and other respiratory illnesses can lead to psychotic episodes. It is very important to pay attention to possible side effects when treating with steroids and evaluate the patient history as well as suggest having a follow up visit after the hospital discharge.
Disclosure of InterestNone Declared
Alternative initiations with 6-monthly paliperidone palmitate. A retrospective study
- S. Benavente López, S. Bolaño Mendoza, A. Parra González, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S488-S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
6-monthly paliperidone palmitate features an initiation regimen through 1-monthly paliperidone palmitate or 3-monthly paliperidone palmitate. Some patients do not have sufficient adherence to treatment and it is necessary at the clinical level to start directly with 6-monthly paliperidone palmitate. There is little clinical experience with these alternative initiations and through this work those that have been carried out for 12 months at the Hospital Universitario Infanta Elena are exposed.
ObjectivesThe main objective of the study is to describe the alternative initiations performed with 6-monthly paliperidone palmitate in routine clinical practice, having opted for a regimen different from the standard for clinical reasons.
MethodsA retrospective selection of patients will be made through non-probabilistic consecutive sampling, including all patients who have been administered 6-monthly paliperidone palmitate with a start different from the standard during the last 4 months. To do this, the electronic medical record will be used, first selecting the patients who have started 6-monthly paliperidone palmitate through the anonymized digital records and, later, including in the study only those who have followed an alternative initiation pattern. The variables studied will be the following: age, sex, diagnosis, dose of paliperidone palmitate, initiation regimen, consumption of toxic substances, absenteeism from 6-monthly paliperidone palmitate, and visits to the emergency room and admissions.
ResultsThe study included a total of 20 patients (n: 20). 80% of the patients were male and 20% were female. The mean age was 39.7 years. 75% of the patients had an associated substance use disorder. The following alternate starting schedules were performed with biannual paliperidone palmitate: monthly paliperidone palmitate on days 1 and 8, and 6-monthly paliperidone palmitate on day 38 (n: 11); monthly paliperidone palmitate 150 mg together with semi-annual paliperidone palmitate both on day 1 (n: 5); biannual paliperidone palmitate on day 1 supplemented with oral paliperidone for 45 days (n:4). A total of 0 visits to the emergency department and 0 admissions were observed after the 6-monthly paliperidone palmitate regimen.
ConclusionsAlternative initiations with 6-monthly paliperidone palmitate may be a useful and safe clinical alternative in patients with very low adherence who, due to clinical needs, require starting 6-monthly paliperidone palmitate earlier in order to guarantee adherence.
Disclosure of InterestNone Declared
Joint treatment of an acute manic episode and a multiple sclerosis debut: A case study
- M. Fariña Francia, E. Marimon Muñoz, E. Miranda Ruiz, I. Fernandez Marquez, R. G. Troyano, J. Ramirez Gonzalez, S. Ferreiro Gonzalez, C. Hidalgo Vazquez, A. Quispe Sulca, M. I. Arroyo Ucar
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S570-S571
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Multiple Sclerosis (MS) is an autoimmune inflammatory disease that affects 1 in 1000 people. Given the association of MS to many affective disorders and specifically with Bipolar Disorder (BD), it is possible that a manic episode and an acute episode of MS may appear together. In these cases, it is difficult to decide whether it is necessary to start a corticosteroid regimen as treatment for the acute episode of MS, since it may worsen manic symptoms.
ObjectivesThe aim is to carry out a review of the existing information in relation to the comorbidity prevalence of MS and TB as well as the joint treatment of both illnesses, and to expose the details of a clinical case, regarding the treatment that was used in the acute psychiatry unit.
MethodsFirst, a search was done in PubMed database reviewing recent cases of steroid induced psychosis using the words (Multiple Sclerosis) AND (Bipolar Disorder). Subsequently, we describe the case of a 41-year-old patient who was admitted to the acute care unit from the emergency department presenting manic symptoms (megalomania, sensation of increased capacities and ideas of mystical content) associated to episodes of muscle weakness and gait disturbances. A screening Magnetic Resonance was performed in which lesions with inflammatory-demyelinating characteristics were detected, and was therefore catalogued as MS debut.
ResultsAfter carrying out a bibliographical review, we can conclude that studies recommend the inclusion of MS within the differential diagnosis of a first manic episode (1), performing neurological examinations, complete anamnesis and imaging tests, given that there is a high prevalence ratio of the comorbidity (2.95%) (2). It has been described that the use of lithium has a calming and neuroprotective agent that may be useful (3).
ConclusionsWe consider it of interest to describe the therapeutic approach to the case. After the introduction of Aripiprazole and Lithium, a short regimen of methylprednisolone in high doses was administered to treat the MS episode. When the treatment started, the patient presented a progressive improvement of the manic episode and motor symptoms. We observed that corticosteroid therapy did not worsen the manic symptoms or the patient’s evolution in this case. We intend to contribute by providing information on the joint management of these pathologies and we consider that it is necessary to continue studying this matter to be able to manage these cases in the most appropriate way.
Disclosure of InterestNone Declared
Clinical experiences with 6-monthly paliperidone palmitate after 12 months of use. A retrospective study
- S. Benavente López, A. Parra González, S. Bolaño Mendoza, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S488
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIA) have provided a significant improvement in the treatment of schizophrenia. Although there is already significant clinical experience with paliperidone palmitate, it is important to evaluate the clinical response of patients to this new 6-monthly presentation, so descriptive studies based on real clinical evidence can be very useful for this purpose.
ObjectivesThe main objective of the study is to describe the use of 6-monthly paliperidone palmitate in routine clinical practice, providing variables that objectify the evolution such as the number of admissions and visits to the emergency room.
MethodsRetrospective descriptive study with a sample selected by non-probabilistic consecutive sampling, retrospective type, in a time interval of 12 months (n=40). The patients selected were all those who received 6-monthly paliperidone palmitate treatment, with a diagnosis of schizophrenia, in 12 months of use at Hospital Universitario Infanta Elena. A descriptive analysis was performed. Mean and standard deviation were calculated for quantitative variables and N and percentage for categorical variables.
ResultsA total of 40 administrations of 6-monthly paliperidone palmitate were performed in the study. None of the patients presented adverse reactions related to the administration of the drug, not reporting local pain or inflammation of the puncture area, except for the characteristic discomfort of an intramuscular puncture. Regarding the efficacy of 6-monthly paliperidone palmitate, none of the patients presented a psychotic decompensation after its administration, maintaining psychopathological stability after the change. The switch to 6-monthly paliperidone palmitate was made from both 1-monthly paliperidone palmitate and 3-monthly paliperidone palmitate, both showing the same efficacy. Regarding tolerability, all the patients who were administered 6-monthly paliperidone palmitate were previously treated with the monthly and quarterly presentation of the same molecule, having presented good tolerability to it, maintaining said tolerability after treatment. change to 6-monthly paliperidone palmitate, with no adverse reaction being recorded after the change. The adherence presented by the patients was very good, performing 100% of the administrations of 6-monthly paliperidone palmitate
Conclusions6-monthly paliperidone palmitate may be an effective and well-tolerated treatment for the treatment of schizophrenia. In the present study, the use of said LAIA in a group of 40 patients is objectified, showing excellent efficacy and tolerability. All study patients were already stable with the 1-monthly and 3-monthly paliperidone palmitate formulations, maintaining said psychopathological stability when switching to the 6-monthly paliperidone palmitate formulation, with excellent adherence and adverse effect profile .
Disclosure of InterestNone Declared
The therapeutic potential of psilocybin in depression resistant to psychotropic drugs
- J. Ramírez González, I. Fernández Márquez, S. Ferreiro González, E. M. Ruíz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S834
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The use of hallucinogens has accompanied the human being throughout history. In the 1970s, studies focused on the therapeutic potential of hallucinogens were blocked due to their misuse in the young population. At present, psilocybin is re-emerging as the center of attention due to its possible therapeutic potential in different psychiatric pathologies such as depression, anxiety or substance use.
ObjectivesThe main objective of this work has been to review recent studies on the therapeutic potential of psilocybin in drug-resistant depressive disorder.
MethodsFor the search for articles, the search strategy “psilocybin AND depression” was established in PUBMED. Regarding the inclusion criteria, it was established that they were recent articles, in Spanish or English and that the full text was freely accessible. On the other hand, those articles whose studies did not focus on humans and resistant depressive disorder were excluded. A total of 19 articles were obtained to review.
ResultsFocusing on Drug-Resistant Depressive Disorder, multiple studies have agreed that the administration of one or two microdoses (10-25mg) of psilocybin accompanied by psychotherapy improves the clinical picture for at least 6 months. These results make us feel optimistic in the search for new treatments in the field of mental health.
ConclusionsPsilocybin microdoses associated with psychotherapy improves depressive symptoms in a patient resistant to common antidepressants.
The psilocybin response in terms of improvement of the depressive symptoms persists after 6 months of evolution.
One or, in some two cases, two microdoses of psilocybin (10-25mg) are enough to obtain statistically significant results in the improvement of the depressive symptoms.
Disclosure of InterestNone Declared
Treatment adherence of a case managed program for patients with severe schizophrenia compared to standard care in mental health units.
- S. Díaz-Fernández, J. J. Fernández-Miranda, F. López-Muñoz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1088-S1089
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Although some studies have reported that case management (CM), when is compared with standard care, reduces the loss of contact with health services, the debate continues about its superiority over other treatment models.
ObjectivesTo assess treatment adherence and reasons for treatment discontinuation, and the impact of the type of APs administration on it, for a group of patients with schizophrenia treated in a CMP or receiving standard treatment in mental health units (MHUs).
MethodsAn observational, longitudinal study (ten-year follow-up) was conducted on 688 patients with severe schizophrenia (CGI-S ≥ 5). All the causes of the end of treatment were recorded, together with the AP medication prescribed and kind of regimes.
Results43.6% of the patients had discontinued treatment in MHUs and only 12.1% on the CMP (p < 0.0001). 27.6% of patients in MHUs were on long-acting injectables (LAIs), and 57.6 on the CMP (p < 0.001). Treatment discontinuation was closely linked to be on OAPs medication in both cases (p < 0.001).
Table 1. Treatment discontinuation, hospital admissions and suicide attempts [N(%)] N= 688 MHU (N=344) CMP (N= 344) P value Treatment discontinuation 290 (84.3) 42 (12.2) <0.00001 OAP LAI OAP LAI Treatment discontinuation 180(52.3) 90(26.2)a 34(9.9) 8(2.3)b Hospital admissions 260 (75.6) 80 (23.5) <0.001 OAP LAI OAP LAI Hospital admissions 180 (52.3) 80 (23.5)a 65 (18.9) 15 (4.4)b Suicide attempts 134 (38.9) 26 (7.7) <0.0001 OAP LAI OAP LAI Suicide attempts 160(46.5) 74(21.5)a 18(5.2) 8(2.3)b a: p<0.01 b: p<0.001 N: number of patients %: percentage of patients
MHU: mental health unit CMP: case managed programme
AP: antipsychotic FGA, SGA: first, second generation antipsychotic
OAP: oral antipsychotic LAI: long-acting injectable antipsychotic
ConclusionsOur findings show how specific strategies as programs with an integrated treatment and case-managed approach, increase adherence. Moreover, treating with LAI APs clearly contributes to the achievement of these results. The widespread implementation of comprehensive community programs with case management, and the use of LAI-APs, should be an effective choice for people with schizophrenia and clinical severity and impairment, and at high risk of treatment discontinuation.
Disclosure of InterestNone Declared
The silent waitress. A case report of mutism without catatonia
- T. Fernández, E. Pujal, S. Salmeron, M. Bioque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S627-S628
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism, defined as an inability or unwillingness to speak, resulting in an absence or reduction of speech, has a wide differential diagnosis. It rarely presents as an isolated disability and often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. Mutism is typically associated with catatonia, usually in schizophrenia, but also depression, bipolar disorder, intoxication, and neurological conditions.
ObjectivesTo describe a case of mutism without catatonia.
MethodsWe describe a clinical case of a patient admitted to our psychiatric inpatient unit with mutism as the presenting symptom. The literature on this subject is also selectively reviewed.
ResultsA 49-year-old woman was found mute at home by her brother and brought to our emergency room. Not a word had come out of his mouth for the past month. She would show up at the restaurant where she worked as a waitress and do her job, but she didn’t talk. As a result, she had been fired. Her routine daily chores and her vegetative functions were maintained. She had no prior history of medical or psychiatric illness or substance abuse. In addition to the mutism, the patient showed an important psychomotor restlessness and performed repetitive hand movements suggestive of occupational delirium. There was no rigidity, stupor, negativism, catalepsy, echosymptoms or any other catatonic symptomatology.
She was then admitted to our inpatient unit, where a complete blood test, EKG, brain CT, brain MRI, EEG and a lumbar puncture with biochemistry and neuroimmunology studies were performed, none of them showing any abnormalities.
The clinical presentation suggested the diagnosis of either a psychotic disorder or a major depressive episode.
The patient was then started on olanzapine up to 20 mg/d, fluoxetine up to 20 mg/d and lorazepam up to 6 mg/d. Due to persistence of symptomatology despite pharmacological treatment, she was started on Electroconvulsive Therapy (ECT). At the time of issuance of this report, 7 bilateral ECT courses have been carried out and absolute mutism persists. Although she has presented an improvement of the anxiety and the repetitive behaviors noted on admission have disappeared, she hasn´t resumed speaking.
ConclusionsMutism occurs in a number of conditions, both functional and organic, and an accurated diagnosis is important for the management. One must perform a thorough physical and systemic examination to rule out organic causes for mutism. An observation for some time period may be warranted and should be done to reach final diagnosis in our case.
Disclosure of InterestNone Declared









